
People with severe mental illnesses (SMI) experience much poorer oral health that the general population with higher rates of tooth loss (Kisely et al., 2015), gum disease and dental decay (Kang et al., 2022).
Interventions developed to improve oral health in people with SMI have not been effective and there is a lack of understanding of barriers and facilitators to engaging with oral health interventions from the perspective of people with SMI, carers and health professionals.
This study led by Mishu and colleagues (2022) aimed to map the contextual factors and behavioural change techniques in existing oral health interventions for people with SMI, and then investigate the current barriers and facilitators at individual, interpersonal and structural levels.

People with severe mental illness suffer much higher levels of dental disease and tooth loss compared to the general population.
Methods
A systematic review of previous behaviour change interventions for improving oral health in SMI was used to extract behaviour change techniques underpinning those interventions. These were then used to prepare video vignettes which were used to conduct qualitative interviews with service users and service providers. Framework analysis was used to summarise the interview data using a coding matrix to produce structured outputs.
The grouping of the barriers and facilitators was reported under the TDF domains. Further grouping of the barriers and facilitators under the TDF (Theoretical Domains Framework) domains according to the COM-B model provided an insight into the capability, opportunity and motivation drivers of behaviour change that can be tapped into to enable the development of interventions that provide integrated support to people with SMI.
Results
Seven service users and ten service providers were interviewed remotely using Zoom, with interviews lasting two hours. There was an equal distribution of genders among participants and the median age was between 31-40 years.
Barriers
Service users reported the following:
- Need for practical help with finding/setting up an appointment with the dentist
- The long waiting list to visit a dentist
- Lack of availability of trauma-informed dentists
- Oral health was not their top priority
- Trust issue with someone new coming in to talk about oral health
- Lack of support after being discharged
Service providers included:
- Need for training around oral health for mental health care staff
- Need for training around mental health and side effects of psychotropic medication for dental health care staff
- Increased workloads
- Lack of availability of integrated care model
- Funding/commissioning issues.
Facilitators
Facilitators for service users included the:
- Involvement of the care coordinators
- Provision of oral hygiene aids such as toothbrushes and toothpaste
Similarly, service providers believed that the following could facilitate accessing oral interventions:
- Involvement of carers and care coordinators
- Use of checklists
- Video demonstrations on oral health self-care.

Lack of communication by the service providers, lack of support in visiting a dentist and long follow-up times act as barriers to accessing oral interventions.
Conclusions
The authors concluded:
The findings suggest that comprehensive interventions that target barriers and enhance facilitators from the individual to systems level are needed to improve the oral health outcomes of people with SMI.
The use of care coordinators and carers can support oral health self-care and dental access among people with severe mental health difficulties. Additionally, video demonstrations and checklists were identified as useful for oral self-care, as were the provision of oral self-care aids like toothbrushes and toothpaste. It’s also important that we move towards integrated services where dental and mental health services can communicate easily and refer patients without unnecessary bureaucracy or financial constraints.

An integrated care model was perceived as the way forward where dental and mental health services are provided under ‘one roof’.
Strengths and limitations
Dental diseases like tooth decay, gum disease and oral cancer are preventable if good oral self-care behaviours are implemented at the outset. We have shown that oral self-care behaviours are worse in people with severe mental illness (Turner et al., 2021). This article has highlighted the barriers and facilitators for the implementation of both self-care and system-level oral health interventions from the point of diagnosis including the provision of toothbrushes, fluoride toothpaste and advice on oral self-care. We, therefore, need to shift our focus from ‘downstream’ treatments that commonly involve the extraction of teeth and are offered in crisis for advanced tooth decay and gum disease, to ‘upstream’ prevention and early intervention when a diagnosis of psychosis is first established.
The strengths included the use of service users from different settings (community and in-patient) which took into account the range of presentations of mental illness severity although numbers could have been better balanced as there was only one interview with a carer and details of health professionals interviewed were unclear. The inclusion of commissioners and policymakers would have been beneficial to explore their views on funding dental services for this patient group, for whom large oral health inequalities exist.

The inclusion of commissioners and policymakers would have been beneficial to explore their views on funding dental services for this population.
Implications for practice
The findings of this recent paper (Mishu et al, 2022) link directly into our recent Oral Health Consensus Statement – The Right To Smile (PDF), which purports a whole team approach right from the start and is supported by the findings of this paper.
The importance of supporting the physical health needs of people experiencing psychosis is now accepted. However, The Right to Smile asserts a ‘whole-person’ approach where there can be no health without oral health. To achieve its goals and targets requires ‘a whole team approach’ that prioritises oral health from the onset of psychosis:
- The patient and their close supporters (e.g. family) must be actively engaged at the centre of the team in discussions about oral health. This was seen to be a facilitator in the findings of the current study(Mishu et al, 2022).
- The mental health practitioner and the team responsible for early diagnosis and treatment should consider oral health needs from the outset. This study found the lack of training of mental health care staff on oral health to be a barrier (Mishu et al, 2022).
- The dental professional must be aware that people with psychosis are a high-risk group for poor oral health and must also be trauma-informed. Perhaps special care dentistry services may be best placed to manage people with severe mental illness, as they have adequate training and time allocation compared with primary care dentists.
It’s time to raise expectations from those using mental health services to receive higher standards of oral healthcare. If we equip people with the right knowledge and skills, while supporting the adoption of healthy routines including regular dental check-ups before things go wrong, we can make a real difference to an individual’s health and well-being.
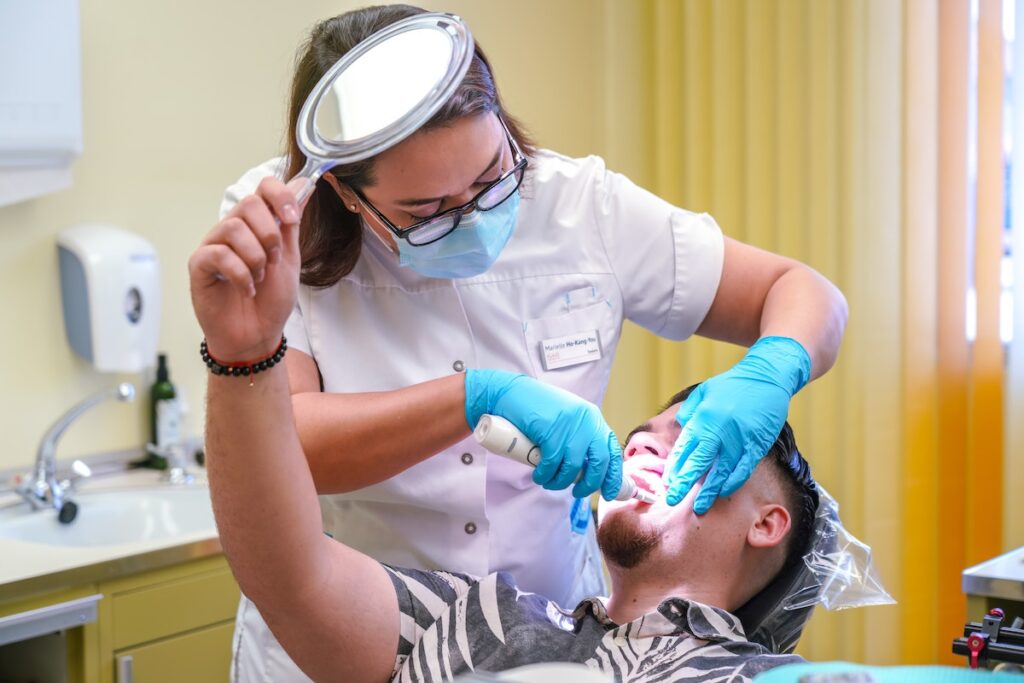
Oral health needs to be included in physical health checks for people with severe mental illness and should be an integral part of care plans.
Statement of interests
None.
Links
Primary paper
Mishu, M. P., Faisal, M. R., Macnamara, A., Sabbah, W., Peckham, E., Newbronner, L., Gilbody, S., & Gega, L. (2022). Exploring the contextual factors, behaviour change techniques, barriers and facilitators of interventions to improve oral health in people with severe mental illness: A qualitative study. Frontiers in Psychiatry, 13, 971328. https://doi.org/10.3389/fpsyt.2022.971328
Other references
Kisely, S., Baghaie, H., Lalloo, R., Siskind, D., Johnson, N.W. A Systematic Review and Meta-Analysis of the Association Between Poor Oral Health and Severe Mental Illness. Psychosom Med. 2015; 77(1): 83–92.
Kang J, Palmier-Claus J, Wu J, Shiers D, Larvin H, Doran T, Aggarwal VR. Periodontal disease in people with a history of psychosis: Results from the UK biobank population-based study. Community Dent Oral Epidemiol. 2022 Oct 18.
Turner, E., Berry, K., Aggarwal, V.R., Quinlivan, L., Villanueva, T., Palmier-Claus, J. Oral health self-care behaviours in serious mental illness: A systematic review and meta-analysis. Acta Psychiatr Scand. 2021
Photo credits
- Photo by Diana Polekhina on Unsplash
- Photo by Enis Yavuz on Unsplash
- Photo by Brian Tromp on Unsplash
- Photo by engin akyurt on Unsplash
