
Obsessive-compulsive disorder (OCD) is a highly prevalent disorder that is associated with a negative impact on quality of life (Macy et al, 2013). It is characterised by individuals experiencing obsessive, unwanted and unpleasant thoughts, images or urges that repeatedly enter a person’s mind, causing feelings of anxiety, disgust or unease (NHS Choices, 2016).
Previous systematic reviews and meta-analyses on the treatment of OCD have used traditional pairwise analytic techniques, which have indicated both efficacy for medication and psychotherapy as effective interventions (Eddy et al, 2004).
This new review recently published in The Lancet Psychiatry seeks to update the evidence base using network meta-analysis, which is increasing being used to assess the relative effectiveness of treatments that may not have been compared in direct trials (Lumely, 2002) and may inform treatment choices of patients and clinicians.

OCD is an extremely debilitating and complex condition, which can leave people feeling hopeless and social isolated.
Methods
- The authors searched the Cochrane Collaboration Controlled Trial Register for common mental disorders, which collates randomised controlled trials (RCTs) from MEDLINE, Embase and PsycINFO
- Trials were included if they were RCTs and included adults with a diagnosis of OCD
- Trials of treatment-resistant patient populations were excluded or if comorbidities were schizophrenia or bipolar disorder
- Interventions included in the review were all antidepressants and psychotherapies recommended by current guidelines
- Eligibility controls were drug placebo or psychological placebo (an intervention that contains non-specific components of therapy) or another non-specific psychotherapeutic relationship
- The Yale Brown Obsessive Compulsive Scale (YBOCS) was used as the primary outcome measure for the network analysis and mean change from baseline was the preferred outcome.
- Pre-planned sensitivity analysis was documented to exclude studies with a high risk of bias and the study protocol was registered on PROSPERO
- Data extraction followed the Cochrane Data Handbook.
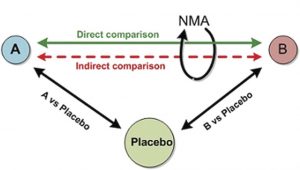
This new network meta-analysis compares the relative effectiveness of various interventions using both direct and indirect evidence.
Results
- 64 trials were included in the qualitative review and 53 trials were included in the network meta-analysis
- The range of antidepressant use in trials ranged between 13-100% and in two-thirds of studies medication use was 45% or higher in the trial. Patients were not allowed to adjust their dosage of medication during the trial, but no study included details of how this was monitored
- The majority of trials in both reviews were North American or European studies.
Network meta-analysis
- The network meta-analysis involved 17 different treatments grouped into various classes:
- All six SRRIs were grouped together
- Clomipramine
- Behavioural Therapy (BT)
- Cognitive Behavioural Therapy (CBT)
- Cognitive Therapy
- Hypericum (St John’s Wort)
- CBT and Fluvoxamine
- BT and Clomipramine
- Most active interventions showed a significant reduction in the mean YBOCS compared with drug placebo
- Venlafaxine and psychological placebo showed reductions but these were not significant
- BT, CBT and CT showed greater efficacy than drug placebo
- However CBT was less effective than BT
- CT and did not differ from psychological placebo
- CBT did show a greater effect when studies using a waiting list control were excluded. When this was done CBT was differentiated from psychological placebo and was similar to BT and CT
- In the full network analysis, BT and CT had larger YBOCS reductions than did SSRIs when grouped as a class
- The differences in all comparisons were small.

This review found that combining an SSRI antidepressant with psychotherapy is possibly the most effective treatment for OCD in adults.
Conclusion
- Several pharmacological and psychotherapeutic interventions are more efficacious that drug placebo
- SSRIs were generally equally effective and clomipramine was not more effective than SSRIs
- CBT had a smaller than expected effect than BT and CT, this was reduced when the waiting list control was excluded, as the comparison condition has been identified with over-estimating the effect sizes from active interventions
- Psychotherapeutic interventions were more effective than medication when considered as a monotherapy
- Given the available evidence, combination treatment of an SSRI antidepressant and psychotherapy is possibly the most effective treatment and should be considered more often, especially with those with serve OCD symptoms.
Strengths and limitations
Overall there were several strengths of the review, such as the inclusion of a large number of trials and the authors conducting a sensitivity analysis excluding waiting list controlled trials, which gives a more accurate estimation of the treatment effect. The strength of a network meta-analytical approach is that it allows the comparison of multiple treatment alternatives simultaneously, some of which may not have been compared directly in primary research studies.
The authors identified several limitations in the review. The majority of the studies did not evaluate efficacy in the long-term, which means that any conclusions can only assess change in the short-term. This is further limited by the older studies reporting only data from treatment completers and as such any treatment effect may be inflated. In addition it was not possible to assess the relative dosage of medication so it is not possible to determine if there is a dosage response and the relative differences between types of medication. Another limitation of the review is the relative effectiveness of psychotherapy or medication as the best monotherapy could not be determined as the majority of trials contained participants who were on a stable dosage medication and therefore the effects cannot be easily separated. The review did not compare the relative efficacy of individual and group treatment.

Individual and group formats of behavioural or cognitive therapies were not compared.
Discussion
This well conducted review employs network meta-analysis techniques to assess the available evidence for psychological and pharmacological treatments. Given the available evidence, the most likely effective treatment is a combination of antidepressant medication and psychotherapy, which is an important point for clinicians to consider when offering treatment for OCD.
It is also the first review to compare the relative effectiveness using both direct and indirect evidence, which is a strength, although trial methodology and transparency of medication reporting are significant limiting factors in making anything other than a tentative and conservative interpretation.
It is further limited by the short-term duration of treatments and the difficulty in determining the impact of dosage on effectiveness or what is the most effective format for psychotherapeutic interventions or which components of therapy are the most effective.

Future research should explore the level of insight that patients have into their condition, the therapeutic relationship, and the impact of family accommodation on symptoms.
Links
Primary paper
Skapinakis P, Caldwell DM, Hollingworth W, Bryden P, Fineberg NA, Salkovskis P, Welton NJ, Baxter H, Kessler D, Churchill R, Lewis G. (2016) Pharmacological and psychotherapeutic interventions for management of obsessive-compulsive disorder in adults: a systematic review and network meta-analysis. The Lancet Psychiatry, Volume 3, Issue 8, August 2016, Pages 730-739, ISSN 2215-0366,http://dx.doi.org/10.1016/S2215-0366(16)30069-4.
Other references
Eddy, K.T., Dutra, L, Bradley, R. & Westen, D. (2004). A multidimensional meta-anaylsis of psychotherapy and pharmacotherapy for obsessive-compulsive disorder. Clinical Psychology Review, 24(8), 1011-1030. [PubMed abstract]
Lumley, T. (2002) Network meta- analysis for indirect treatment comparisons. Statistics in Medicine, 21(16), 2313-2324. [Abstract]
Macy, A.S., Theo, J.N., Kaufmaunn S.C et al. (2013) Quality of Life in obsessive compulsive disorder. CNS Spectrums, 18, 21-33. [PubMed abstract]
NHS Choices (2016) Obsessive Compulsive Treatment (OCD) http://www.nhs.uk/conditions/Obsessive-compulsive-disorder/Pages/Introduction.aspx

Antidepressants and psychotherapy for OCD in adults: network meta-analysis https://t.co/ehion8I2fB #MentalHealth https://t.co/dwUkIQ8sGg
Today @weeal36 on recent @TheLancetPsych network meta-analysis of medication & talking treatments for #OCD https://t.co/QPGamKes4U
#Antidepressants & #psychotherapy for #OCD in adults: network #metaanalysis https://t.co/Kl6wwq1kPw
Antidepressants and psychotherapy for OCD in adults: network meta-analysis https://t.co/qUBRW9A4pj via @sharethis
Combining antidepressants & psychotherapy
May be most effective treatment for OCD in adults
https://t.co/Xm98AezNWa https://t.co/TnNHBsS195
Don’t miss;
Antidepressants and psychotherapy for #OCD in adults
Network meta-analysis
https://t.co/QPGamKes4U https://t.co/NHeFq5Upn5
[…] Antidepressants and psychotherapy for OCD in adults: network meta-analysis – (2016) Pharmacological and psychotherapeutic interventions for management of obsessive … […]